What is Thrombophilia?
Thrombophilia is a common blood clotting problem that can have life-threatening consequences.
Find out if you are at risk - get tested
| Test Type | Testing Time | Fee |
| 4 to 6 weeks | $195 Click Here to Order Kit |
All orders received before 3pm PST / 6pm EST are shipped out the same business day. All orders received after 3pm PST / 6pm EST or on weekends or holidays are shipped out the following business day. 24/7 online status check and account management available for all tests.
What is Thrombophilia?
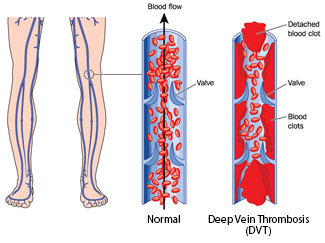
Thrombophilia is a condition where the blood has an increased tendency to form clots. A blood clot within a vein is known as venous thrombus and the most common form is deep vein thrombosis, which is a blood clot in the deep veins of the leg. If this blood clot breaks loose and travels to the lungs, it is known as pulmonary embolus and can be very dangerous. A less common (and more severe) form of venous thrombus is known as cerebral venous sinus thrombosis, where a blood clot forms in the dural venous sinuses, which drain blood from the brain.
What are the Risk Factors for Thrombophilia?
Abnormal blood clotting can occur in anyone but there are certain things that increase the chance of this potentially fatal problem. The more risk factors that an individual has, the higher the chance of a blood clot. Some risk factors cannot be changed and these include age-related risk, ethnic background and genetic risk factors.
The risk of blood clotting for children under 15 years is less than 1 in 20,000, but those in their fifties have a 1 in 760 to 1600 chance of a blood clot. Elderly people (over 80 years of age) have an even higher risk, with about 1 in 170 to 220 suffering from a blood clot. Some ethnicities have an increased risk of thrombophilia compared to others. African Americans have the highest risk, followed by Caucasians and Hispanics. Asians and Pacific Islanders have a much lower risk but blood clots can still occur.
Some genetic mutations can also increase the risk of thrombophilia. These mutations can be passed from generation to generation and cause ‘inherited thrombophilia’. The thrombotic risk DNA panel offered here includes the analysis of mutations in three genes – F5, F2 prothrombin and MTHFR – that all increase the risk of thrombophilia.
There are several health, environmental and lifestyle risk factors that also contribute to thrombophilia, including surgery, injury, infections and inflammatory disease. Each of these increases the chance of blood clots to varying degrees and the associated trauma and immobility play a role in the chance of thrombophilia. Diabetes, cancer and cancer treatments can also increase the risk of thrombophilia. Some risk factors, such as a sedentary lifestyle, obesity and smoking can be reduced by lifestyle changes.
Hormone changes from contraceptive pills and hormone replacement therapies or during pregnancy can all increase the risk of thrombophilia to varying degrees. Contraceptive pills and hormone replacement therapy (to relieve menopause symptoms) increase the risk of abnormal blood clots by 2- to 4-fold and, if combined with one or more of the genetic mutations described above, the risk can be up to 100 times higher compared to someone without the same risk factors.
Pregnancy also increases the risk of abnormal blood clotting by approximately 4-fold. Thrombophilia may also increase the chance of other pregnancy complications including preeclampsia (high blood pressure and proteinuria), placental abruption (placenta tears from uterus wall), reduced fetus growth and recurrent miscarriages.
High homocysteine levels in the blood can also contribute to abnormal blood clotting. There are two mutations in the MTHFR gene that can lead to high homocysteine levels, but other factors also play a role. Many of these are the same as the risk factors described above, including cancer, diabetes, smoking and older age. Other risk factors for increased homocysteine levels include a Vitamin B deficiency, reduced kidney, liver or thyroid function, increased blood pressure, certain drugs and too much coffee.
Next, Signs and Symptoms of Thrombosis »
Recommended Links: Gatt A, Makris M. Hyperhomocysteinemia and venous thrombosis (2007). Semin Hematol. 44(2): 70-6.
