How is Thrombophilia Prevented or Treated?
Reducing your risk of life-threatening blood clots
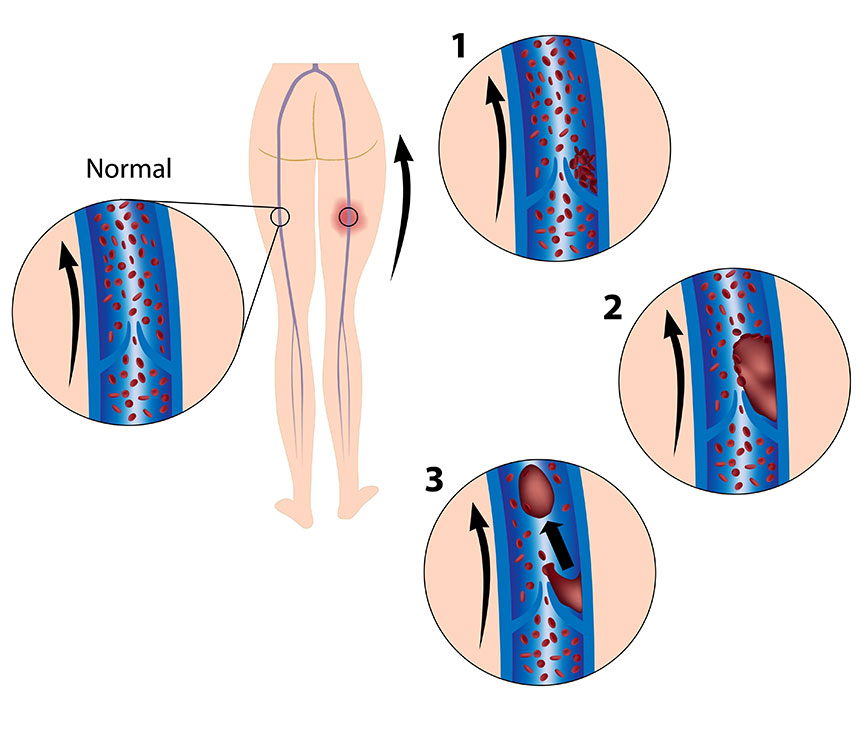
Find out if you are at risk - get tested
| Test Type | Testing Time | Fee |
| 4 to 6 weeks | $195 Click Here to Order Kit |
All orders received before 3pm PST / 6pm EST are shipped out the same business day. All orders received after 3pm PST / 6pm EST or on weekends or holidays are shipped out the following business day. 24/7 online status check and account management available for all tests.
Reducing the Risk of Thrombophilia
Although some risk factors (e.g. genetics and age-related risk) cannot be changed, there are several others that can be reduced. Extended periods of immobility are a significant risk factor and can often be reduced. After an injury, surgery or an illness, you should move around again as soon as possible to get blood flowing normally. Long trips, particularly air travel, increase the risk of thrombophilia so an effort should be made to get up and move around when possible, exercise your legs by moving feet around to increase blood flow and drink plenty of non-alcoholic fluids. For many people who have already suffered from a blood clot or are at a high risk, compression stockings or medication may also be required.
Hormone changes due to birth control pills and hormone replacement therapy can increase the risk of blood clots; so avoiding these treatments may be necessary for those who have a high risk of blood clotting.
A sedentary lifestyle and obesity also significantly increase the risk of thrombophilia so a weight loss program is a good start for those that are significantly overweight. Physical activity helps maintain a healthy weight and increases blood flow – both important factors to reduce the risk of thrombophilia.
If an individual has high homocysteine levels either due to mutations in the MTHFR gene or other factors (e.g. diabetes, cancer, smoking), supplementation with folate and other B vitamins may help reduce the homocysteine and the associated risk of abnormal blood clots. Generally a well-balanced diet provides enough folate, vitamin B6 and vitamin B12, but taking typical vitamin supplements are also usually safe.
Treating Thrombosis
Anticoagulants are the main treatment for abnormal blood clots. These blood-thinning drugs can also be used as a preventative measure for those with a very high risk of thrombophilia, however long-term use is uncommon, as anticoagulants can have serious side effects.
The aim of anticoagulants is to prevent the blood clot from getting any larger and to stop it breaking loose and traveling to the lungs to cause a pulmonary embolism. Anticoagulants lower the blood’s ability to clot rather than dissolving the original blood clot. With the prevention of further clotting, the blood clot dissolves naturally over time.
The two most common anticoagulants are heparin and warfarin. Heparin is administered via an injection or IV and works very quickly. Warfarin is in a pill form and takes a few days to work effectively but is better for extended treatment after a blood clot. Anticoagulants are generally prescribed for 3 – 6 months after a deep vein thrombosis but can be for extended periods if the patient has a very high risk or has a history of abnormal blood clots. Anticoagulants can have side effects, particularly an increased risk of abnormal bleeding, hence must be monitored carefully.
Next, About the Thrombotic Risk DNA Test »
Recommended Links: McGlennen RC, Key NS (2002). Clinical and laboratory management of the prothrombin G20210A mutation. Arch Pathol Lab Med. 126(11): 1319-25.
